Many stroke patients suffer from significant cognitive decline throughout the subsequent year after a stroke. The new therapy is primed to address that secondary injury
Ayush Batra
Mouse Model Tests Stroke Therapy in Realistic Conditions
The findings are highly relevant for future clinical applications because the scientists tested the approach in a mouse model that closely mimics real-world ischemic stroke treatment, Batra said. They first blocked blood flow to simulate a major ischemic stroke and then restored it (a process called reperfusion), just as doctors restore blood flow acutely for ischemic stroke patients.
“Dancing Molecules” Reduce Brain Damage and Inflammation
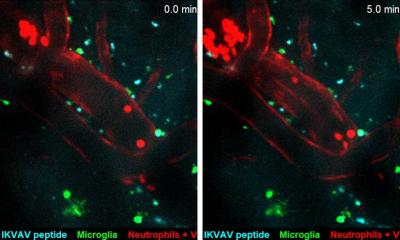
The scientists monitored the mice for seven days and didn’t observe any significant side effects or biocompatibility issues such as toxicity or immune system rejection. They used advanced imaging techniques, such as real-time intravital intracranial microscopy seen in this video, to confirm the therapy localized to the stroke injury site. Compared to untreated mice, those treated with the “dancing molecules” had significantly less brain tissue damage, reduced signs of inflammation and reduced signs of excessive, damaging immune response.
Regenerative and Anti-Inflammatory Effects of the Therapy
Stupp said the therapy has pro-regenerative and anti-inflammatory properties, both of which contributed to the positive results. “You get an accumulation of harmful molecules once the blockage occurs and then suddenly you remove the clot and all those ‘bad actors’ get released into the bloodstream, where they cause additional damage,” Stupp said. “But the dancing molecules carry with them some anti-inflammatory activity to counteract these effects and at the same time help repair neural networks.”
How the ‘Dancing Molecules’ Help Repair Nerve Cells
The secret behind Stupp’s “dancing molecules” breakthrough therapeutic is tuning the collective motion of molecules, so they can find and properly engage constantly moving cellular receptors. The treatment sends signals that encourage nerve cells to repair themselves. For example, it can help nerve fibers (called axons) grow again and reconnect with other nerve cells, restoring lost communication. This process is called plasticity, which means the brain and spinal cord can adapt and rebuild connections after injury.
Nanofiber Technology Helps Therapy Cross the Blood-Brain Barrier
In previous studies, scientists injected the dancing molecules as a liquid, and when used to treat spinal cord injury, the therapy immediately gels into a complex network of nanofibers that mimic the dense, extracellular matrix of the spinal cord. By matching the matrix’s structure, mimicking the motion of biological molecules and incorporating signals for receptors, the synthetic materials are able to communicate with cells. In the new study, the scientists dialed down the concentration of supramolecular peptide assemblies to prevent possible clotting as the therapy enters the bloodstream. Smaller aggregates of peptides easily crossed the blood-brain barrier. Once enough molecules cross, larger nanofiber assemblies can form in brain tissue to produce a more potent therapeutic effect, Stupp said. “We chose for this stroke study one of the most dynamic therapies we had in terms of its molecular structure so that supramolecular assemblies would have a better probability of crossing the blood-brain barrier,” Stupp said.
New Therapy Could Overcome a Major Neuroscience Challenge
The fact that seemingly effective therapies cannot cross the blood-brain barrier has plagued the neuroscience field for decades, Batra said. This new therapy could change that. When a physician acutely restores blood flow to a region of the brain in a stroke patient, the blood-brain barrier permeability is locally increased, naturally creating a transient opening and opportunity for therapeutic intervention, Batra said. “Add to that a dynamic peptide that is able to cross more readily, and you’re really optimizing the chances that your therapy is going where you want it to go,” Batra said.
Future Research Aims to Improve Long-Term Stroke Recovery
Further studies will need to assess whether this treatment can support longer-term, functional recovery, Batra said. For instance, many stroke patients suffer from significant cognitive decline throughout the subsequent year after a stroke. The new therapy is primed to address that secondary injury, Batra said, but the studies will require a longer follow-up period and more sophisticated behavioral testing. In addition, the team is interested in testing whether additional regenerative signals could be incorporated into the therapeutic peptides to produce even better results.
Study Details and Research Support
The study is titled, “Toward Development of a Dynamic Supramolecular Peptide Therapy for Acute Ischemic Stroke.” Graduate student Zijun Gao and postdoctoral researcher Luisa Andrade da Silva are co-first authors of the paper. Funding for this study was primarily provided by the SQI Synthesizer Grant Program at the Center for Regenerative Nanomedicine.
Source: Northwestern University